Daijiworld Media Network - Islamabad
Islamabad, Apr 23: Pakistan is grappling with one of the highest burdens of Hepatitis C in the world, a situation widely attributed to unsafe healthcare practices and the unchecked spread of unqualified medical providers, according to a recent report.
An editorial in The Express Tribune highlighted that nearly 9.8 to 10 million people in the country are living with Hepatitis C. When combined with Hepatitis B cases, the total number of affected individuals rises to an estimated 13.8 to 15 million. Alarmingly, only about a quarter of those infected are aware of their condition.
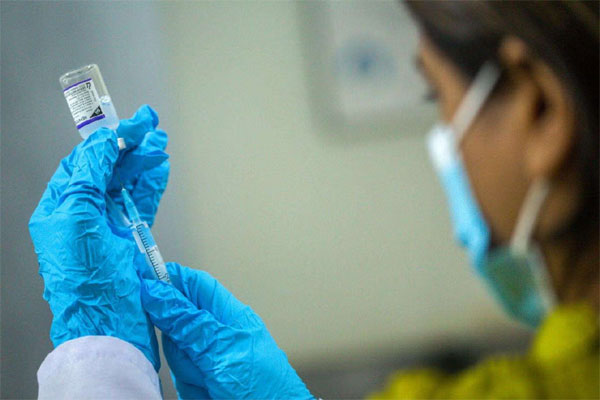
The report pointed to widespread medical negligence as a key factor behind the crisis. Practices such as the reuse of syringes, unsafe blood transfusions, and inadequate sterilisation remain common, often exposing patients to life-threatening infections during routine medical visits. The presence of more than 600,000 unlicensed practitioners—commonly referred to as quack doctors—has further exacerbated the problem.
Hepatitis C primarily targets the liver and can remain undetected for years, often surfacing only after significant damage has occurred. This delayed diagnosis increases the risk of complications such as liver failure and cancer. Limited access to affordable healthcare and low awareness levels make early detection and treatment even more challenging.
In response, Pakistan launched a national programme in 2025 aimed at eliminating Hepatitis C by 2050. However, concerns have been raised about inconsistent implementation and a pattern of short-lived enforcement efforts.
A separate investigation by BBC exposed serious lapses in infection control at a government hospital in Punjab province. The probe, conducted by BBC Eye Investigations, revealed unsafe practices in a children’s ward, including the reuse of contaminated syringes, improper handling of medical waste, and the involvement of untrained personnel in administering injections.
The investigation was linked to an outbreak of HIV at the Tehsil Headquarters Hospital, where at least 331 children tested positive between November 2024 and October 2025. Despite earlier government assurances of a crackdown and administrative action, the report found that unsafe practices continued months later.
The findings underscore deeper systemic issues, including staff shortages, inadequate supplies, and pressure on healthcare workers, which often lead to compromised safety standards. In some cases, families were reportedly asked to procure their own medicines, further complicating treatment.
The situation highlights an urgent need for stricter regulation, improved healthcare infrastructure, and sustained policy enforcement to curb the spread of infectious diseases and restore trust in the medical system.